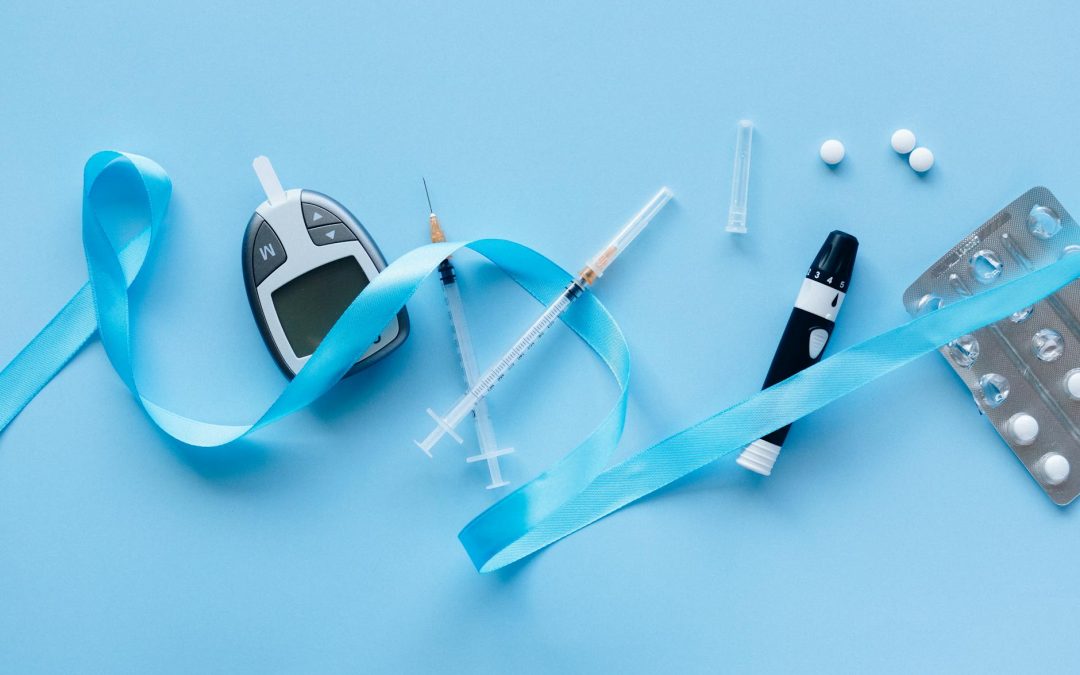
With medical advances extending lifespans for people with type 1 diabetes into their sixties and beyond, you’re probably wondering about the long-term impacts on your health. Xiang Qi from the NYU Rory Meyers College of Nursing highlights the striking magnitude of this increased dementia risk. Most prior studies only focused on type 2 diabetes, or just grouped all diabetes types together, but this research finally fills that important evidence gap, showing you just how much more susceptible you might be.
Let’s look at the numbers: Is the risk really that much higher?
You might be wondering if these links are just a small blip or something you really need to pay attention to. Well, the data from a pretty massive study gives us some clear answers. We’re talking about numbers that really highlight how significant this connection is, especially for those living with type 1 diabetes.
This isn’t just some small-scale observation; the findings are quite striking. You’ll see that the difference in risk isn’t just a slight bump, but a considerably higher chance of developing dementia, and that’s something we should definitely be discussing.
Breaking down the All of Us research data
Many folks assume smaller studies are less reliable, but this research definitely isn’t small-time. The study pulled data from over 275,000 adults, all aged 50 and older, participating in the “All of Us” health research program. That’s a huge pool of information to work with.
Researchers followed these participants for about 2.5 years on average, using their electronic health records. Out of that massive group, about 2,000 people actually developed dementia during the study period.
* Analyzed over 275,000 adults, ages 50 and older.
* Participants from the All of Us health research program.
* Followed for an average of 2.5 years using electronic health records.
* Approximately 2,000 participants developed dementia.
Assume that such a large sample size lends considerable weight to the study’s conclusions.
| All of Us Research Program: Key Figures | |
|---|---|
| Total Adults Analyzed (50+) | 275,000+ |
| Average Follow-up Period | 2.5 years |
| Participants Who Developed Dementia | ~2,000 |
Comparing type 1 and type 2 risk factors
It’s common to lump all diabetes together, but this study really shows us the difference in risk between type 1 and type 2. Among the participants, 5,000 had type 1 diabetes, and a much larger group of 50,000 had type 2 diabetes.
You know, after adjusting for things like age and how much education someone had, the numbers are pretty stark. Type 1 diabetes was linked to an almost three times higher dementia risk, while type 2 also increased the risk, but not quite as dramatically.
* 5,000 participants had type 1 diabetes.
* 50,000 participants had type 2 diabetes.
* After accounting for age and education, type 1 diabetes was linked to 2.7 times the dementia risk compared to no diabetes.
* Type 2 diabetes was linked to 1.7 times the dementia risk compared to no diabetes.
Assume that these adjusted figures give us a clearer picture of the independent impact of each diabetes type.
| Dementia Risk Comparison (vs. No Diabetes) | |
|---|---|
| Type 1 Diabetes | 2.7 times higher risk |
| Type 2 Diabetes | 1.7 times higher risk |
The real deal: Why’s this actually happening to the brain?
You’re probably wondering what’s really going on inside your head, right? Well, it turns out diabetes messes with your brain’s blood vessels, and that vascular damage significantly increases your dementia risk. It’s a complex picture, involving things like hypoglycemia, hyperglycemia, and insulin resistance.
It’s fascinating to consider that type 1 and type 2 diabetes might even affect your brain in *different* ways when it comes to dementia. Michal Schnaider Beeri from Rutgers University points out that all forms of diabetes impact brain blood vessels, which is a pretty big deal for your overall health.
The role of vascular damage and blood vessels
Your brain’s blood vessels are super important, you know? They’re like the highways delivering everything your brain needs. When diabetes affects these vessels, you get vascular damage, and that’s a direct pathway to a higher dementia risk.
Michal Schnaider Beeri of Rutgers University made it clear that every single type of diabetes impacts these crucial brain blood vessels. So, whether it’s type 1 or type 2, your brain’s vascular health is on the line.
How blood sugar swings impact the brain
Imagine your brain trying to function with wild swings in its fuel supply – that’s what happens with blood sugar. Both hypoglycemia (low blood sugar) and hyperglycemia (high blood sugar) are biological mechanisms directly linked to how diabetes contributes to dementia development.
Insulin resistance also plays a role in this brain chemistry rollercoaster. These constant fluctuations and the body’s struggle with insulin can really take a toll on cognitive function over time, making it harder for your brain to do its job.
These dramatic shifts in blood sugar, whether too high or too low, don’t just feel bad; they actively contribute to the brain’s decline. Your brain thrives on stability, and diabetes often prevents that, creating an environment ripe for cognitive issues down the line.

My take on the catch: Some things to keep in mind
These findings, while certainly eye-opening, aren’t the whole story, you know? It’s important to understand the nuances and limitations of any study, especially one drawing conclusions about something as complex as brain
You might be thinking this study proves a direct cause-and-effect relationship, but that’s not quite right. While it *does* add to the growing evidence that metabolic diseases can have long-term effects on brain
Limitations of using electronic health records
Wondering how they got all this info? The study primarily relied on electronic
Sometimes, diagnoses in these records can be less precise, and survey data can be subjective, right? So, the way disease status was determined could introduce some limitations into the overall findings.
The impact of frequent medical checkups
Another interesting point to consider is how often folks with type 1 diabetes see their doctors. They typically have more frequent
This increased medical attention could actually mean that cognitive decline in individuals with type 1 diabetes is simply detected earlier. Think about it – if you’re at the doctor more often, there are more opportunities for someone to notice subtle changes, maybe even before they become really noticeable to the individual or their family.
So, it’s not necessarily that they’re experiencing *more* decline, but perhaps that their decline is just being picked up on sooner due to those regular check-ins. This earlier detection could potentially skew the statistics, making it seem like the risk is higher, when it’s really about the frequency of observation.

So, what’s the best way to stay on top of this?
Protecting your cognitive health means you’ve got to be on your game with managing blood sugar, blood pressure, and cholesterol. For folks with type 1 diabetes, keeping an eye out for those subtle, early cognitive changes is super important, especially since they can mess with how well you stick to your treatment plan.
You see, if a decline in cognitive health goes unnoticed, it can kick off this really nasty cycle: poorer diabetes management, unstable metabolism, and then, boom, accelerated vascular damage. Nobody wants that, right?
Daily management of blood sugar and pressure
Staying on top of your daily blood sugar and blood pressure isn’t just about feeling good today; it’s about safeguarding your brain for tomorrow. You’re crucially building a shield against future cognitive issues by keeping these numbers in check.
Think of it like this: every time you manage your blood sugar and pressure well, you’re investing directly into your long-term cognitive health. It really does make a massive difference.
Breaking the negative cycle of cognitive decline
Catching those first hints of cognitive change is like finding a small leak before it floods the house. People with type 1 diabetes need to be extra vigilant, because early signs can easily be dismissed, but they might be impacting how you manage your diabetes.
Ignoring these changes? That’s where things can get really tricky and dangerous. An unrecognized decline can lead to a downward spiral: worse diabetes management, then metabolic instability, and accelerated vascular damage.
This negative cycle is a big deal, creating a domino effect where poor diabetes control makes cognitive health worse, and a decline in cognitive health makes diabetes management harder. It’s a feedback loop we absolutely want to interrupt.
Conclusion
Following this, you can see why understanding the link between type 1 diabetes and dementia is so incredibly important, especially with people living longer and longer. Individuals with type 1 diabetes really do face a significantly higher rate of dementia, something study coauthor Jennifer Weuve made clear. This isn’t just some academic finding; it’s evidence that should shape future research, clinical health awareness, and even how you plan care and prevention.
So, what does this all mean for you or someone you know? It means you’ve got to prioritize good health management, focusing on both diabetes and brain health. Thinking about these connections now can really make a difference down the road, don’t you think?
Health FAQ: Type 1 Diabetes and Dementia Risk
Q: What’s the big deal with Type 1 Diabetes and dementia risk? I thought Type 2 was the one everyone worried about.
A: You know, for a long time, most of the talk about diabetes and brain health really focused on Type 2. It’s what the research seemed to highlight most often. But new findings are shining a really bright light on Type 1 diabetes, and it’s pretty eye-opening. A recent study, which looked at over 275,000 adults, found that people with Type 1 diabetes actually have nearly three times the risk of developing dementia compared to folks without diabetes. That’s a huge jump, right? It just shows we’re starting to understand the full picture as people with Type 1 live longer and longer, thanks to medical advances.
This study also found that Type 2 diabetes increases the risk, but it’s more like 1.2 times the risk. So, while both are concerning, the connection for Type 1 is significantly higher. It means we can’t just group all diabetes together anymore when we’re thinking about long-term brain health. Researchers are starting to think that the ways Type 1 and Type 2 contribute to dementia might even be different, which is a pretty important distinction for future research and how we approach care.
Q: How does Type 1 diabetes actually increase the risk of dementia? What’s going on in the body?
A: It’s a really complex question, and scientists are still working to figure out all the pieces, but there are some strong theories. One big factor is how diabetes affects your blood vessels, including the tiny ones in your brain. All forms of diabetes can damage these vessels, and that kind of vascular damage definitely increases your risk of dementia. Think of it like this: if the roads to your brain aren’t in good shape, things aren’t going to flow as they should, you know?
Beyond that, there are other biological mechanisms at play too. We’re talking about things like chronic inflammation, which is when your body’s immune system is constantly on alert. High blood sugar levels, even if they’re managed pretty well, can still cause issues over time, leading to inflammation and oxidative stress – basically, damage at a cellular level. Plus, insulin resistance, which can happen even in Type 1 diabetes, might also be a factor. All these things together can create an environment that’s just not great for long-term brain health.
Q: Okay, so if I have Type 1 diabetes, what can I do to protect my brain health and reduce this risk?
A: It’s totally understandable to feel a bit concerned, but the good news is there are concrete steps you can take. The most important thing is to manage your Type 1 diabetes really carefully. This means keeping your blood sugar levels as stable as possible – avoiding those big swings, both high and low. Regular check-ups with your healthcare team are a must, of course, to make sure your treatment plan is working for you.
Beyond that, a healthy lifestyle is your best friend. That means eating a balanced diet, getting regular physical activity, and keeping an eye on your blood pressure and cholesterol levels, as these can also affect your brain’s health. And here’s something really important: pay attention to any subtle changes in your cognitive abilities. If you or your loved ones notice you’re having more trouble remembering things, solving problems, or sticking to your diabetes treatment plan, tell your doctor right away. Catching cognitive decline early can help prevent a negative cycle where poorer diabetes management leads to more damage, which then speeds up further decline. It’s all connected, so being proactive is key!